Learn about the most important sexually transmitted diseases in virtual times and epidemic times
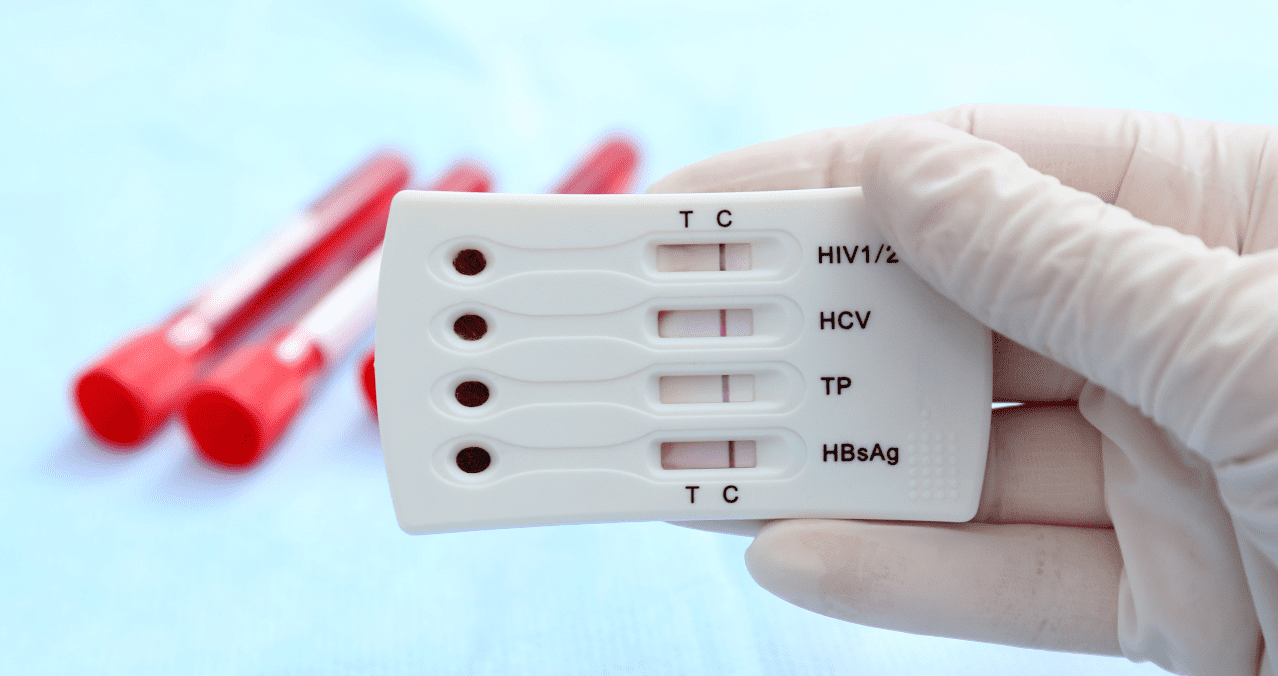
The incidence of gonorrhea and syphilis increased, while the incidence of chlamydia decreased.
Medical examination for HIV, hepatitis B and C and syphilis. Photo: shutterstock.
Reported cases of STIs in the United States declined during the early months of the COVID-19 pandemic in 2020, but most reported STIs increased again at the end of the year.
In the end, cases gonorrheaReported syphilis and congenital syphilis exceeded 2019 levels, while chlamydia cases decreased, according to new data released today from the Centers for Disease Control and Prevention (CDC). The data provides the clearest picture yet of the impact of COVID-19 on the STD epidemic in the United States.
The recently released 2020 STD Surveillance Report found that at the end of 2020:
cases gonorrhea Primary and secondary syphilis increased by 10% and 7%, respectively, compared to 2019.
Syphilis Among newborns (that is, congenital syphilis) also increased; Reported cases increased by approximately 15% from 2019 and 235% from 2016. Preliminary data indicate that cases of primary, secondary and congenital syphilis also continued to increase in 2021.
Historically, chlamydia accounts for the largest proportion of sexually transmitted infections reported in the United States. The decrease in the number of reported cases of chlamydia is likely due to less screening and less diagnosis during a pandemic, rather than a decrease in new infections. This has also contributed to an overall decrease in the number of STIs reported in 2020 (from 2.5 million reported cases in 2019 to 2.4 million in 2020).
“The COVID-19 pandemic has placed enormous pressures on an already stretched public health infrastructure,” said Jonathan Mermin, MD, MPH, director of the National Center for HIV, Viral Hepatitis, STIs, Tuberculosis, and Prevention of COVID-19. . “There were times in 2020 that the world seemed to have stopped, but STDs did not. The ongoing momentum of the STD epidemic continued while STD prevention services were disrupted,” he explained.
Several factors likely contributed to the initial decline in reported STI cases in the first part of 2020, including:
* Decreased in-person healthcare services, due to fewer routine visits, resulting in fewer sexually transmitted tests;
*Reallocation of public health personnel from STI work to COVID-19 pandemic response activitiespdf icon;
* Shortage of STD testing and laboratory supplies; Interruptions in health insurance coverage due to unemployment, and
* Telemedicine practices that led to the failure to record some infections in the national data.
While STDs are on the rise in many groups, 2020 STD data shows that some racial/ethnic minority groups, gay and bisexual men and young adults in our country still have higher rates of STDs. This trend shows that old factors such as lack of access to regular health care and discrimination and stigma still stand in the way of quality sexual health care for all who need it.
“The COVID-19 pandemic has raised awareness of a reality we have known about STDs for a long time. Socioeconomic factors, such as poverty and lack of health insurance, create barriers and increase health risks and often translate into worse health outcomes for some people,” said Leandro. Mina, MD, MPH, director of the CDC’s Division of Sexually Transmitted Diseases Prevention. “If we are to make lasting progress against STDs in this country, we need to understand the systems that create inequality and we need to work with partners to change those systems. No one can be left behind,” he added.
Much remains to be done to restore, renew, and expand STI prevention and control in the United States, and it will require many groups working together, such as health care systems, medical centers, and community-based organizations; public and private sectors; Health care providers and health workers.
Efforts must be prioritized and focused to make up for lost STIs. The outward vision of the United States as a place where STIs are prevented and where everyone has access to high-quality STIs prevention, care, and treatment services that are free from stigma and discrimination could become a reality in the National STI Strategic Plan. Help collaborators and design many people.
Consulting resource over here.

“Award-winning zombie scholar. Music practitioner. Food expert. Troublemaker.”


/cloudfront-eu-central-1.images.arcpublishing.com/prisa/AHVYMMDSTZDTDBFNZ3LMFUOKNE.jpg)