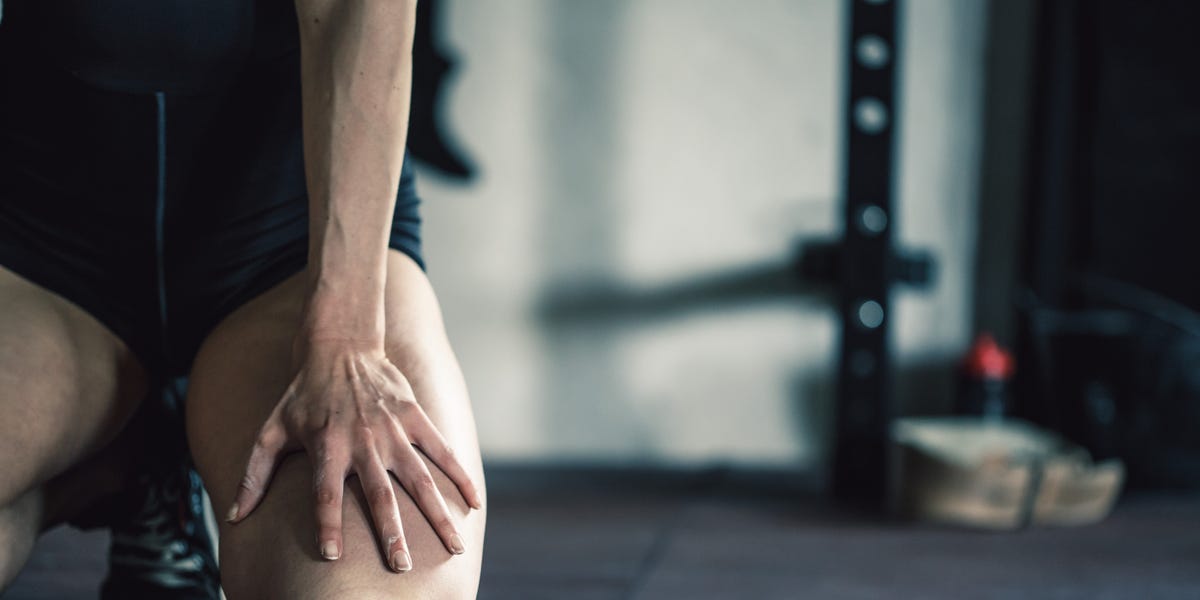
The Puerto Rican study supports the benefits of Mediterranean nutrition in an obese population

Dietary intake was assessed using a food frequency questionnaire with different scales.
Dr. Josemer Mattei, Donald and Sue Pritzker Associate Professor of Nutrition in the Department of Nutrition, Harvard T.H. Chan School of Public Health. Photo: Introduction to the Journal of Medicine and Public Health.
Older adults in Puerto Rico have a high burden of cardiovascular disease, due to marked cardiovascular risks, including obesity, including that prevalent in the abdominal region, which is today associated with metabolic syndrome.
The health burden of these particular diseases is reflected every day in the increasing mortality rate among patients due to these chronic conditions associated with obesity.
For this reason, a group of researchers from the country conducted a study to assess the relationship between Mediterranean Nutrition (MeDS) and the 2010 Alternative Healthy Eating Index (AHEI) – a tool that allows assessment of the eating pattern of populations under the US Dietary Guidelines for Americans – with obesity central in the study’s evaluation. A cross-section of the diet, lifestyle and disease of Puerto Rico (PRADLAD).
The team analyzed data from PRADLAD participants aged 30-75 years in a sample of 166 patients. Dietary intake was assessed using a food frequency questionnaire with different scales, and waist circumference measurements were also taken into account.
Among the most notable findings, it was found that traditional foods representative of the MeDS diet – this diet can vary between populations – including potatoes, tubers, fruit juice, avocados, bread, oatmeal, beans, chicken, seafood, low-fat milk, cheese, eggs, beer and this greater adherence to MeDS or AHEI was associated with lower central obesity in adults in Puerto Rico.
Part of the study’s conclusion reads that, “Consumption of traditional foods that reflect these dietary patterns (i.e., Mediterranean type) can reduce central obesity in high-risk populations.”
This research is the first study to establish and evaluate a MeDS diet adapted to a Puerto Rican population. Data from it can be used for future assessments and nutritional analyzes on the island, given the lack of epidemiological studies in this area.
Among the inclusion criteria were study participants living in Puerto Rico for at least 10 months at the time of the study, answering questions without assistance, and the study was part of an alliance between Harvard T.H. Chan School of Public Health, Ponce. University of Health Sciences, University of Massachusetts Lowell, and Northeastern University.
access to study over here.

“Award-winning zombie scholar. Music practitioner. Food expert. Troublemaker.”


/cloudfront-eu-central-1.images.arcpublishing.com/prisa/AHVYMMDSTZDTDBFNZ3LMFUOKNE.jpg)